Built to make learners decide
The tools here are proof of concept as much as they are finished products. Each one started with a specific teaching problem: a concept that wasn't landing, a case study that deserved more than a lecture slide, a skill that could only be built through practice. The interactive architecture came from asking what it would actually take for a learner to feel the tradeoff, not just understand it.
These tools have been used in postgraduate classrooms and professional training settings, and adapted for different regional contexts and audience levels. All are free to use for non-commercial teaching and training purposes. Most are adaptable — to different contexts, audiences, and settings — and the list of problems that deserve this kind of treatment is much longer than what's here so far.
Strategic Outbreak Response Simulation
A multiplayer simulation in which teams navigate a novel outbreak across six escalating phases — from an unknown pathogen with limited data, through transmission confirmation, peak pressure, public fatigue, and transition to recovery. Each phase presents a menu of non-pharmaceutical interventions with real tradeoffs across health outcomes, economic impact, community trust, equity, and resource constraints.
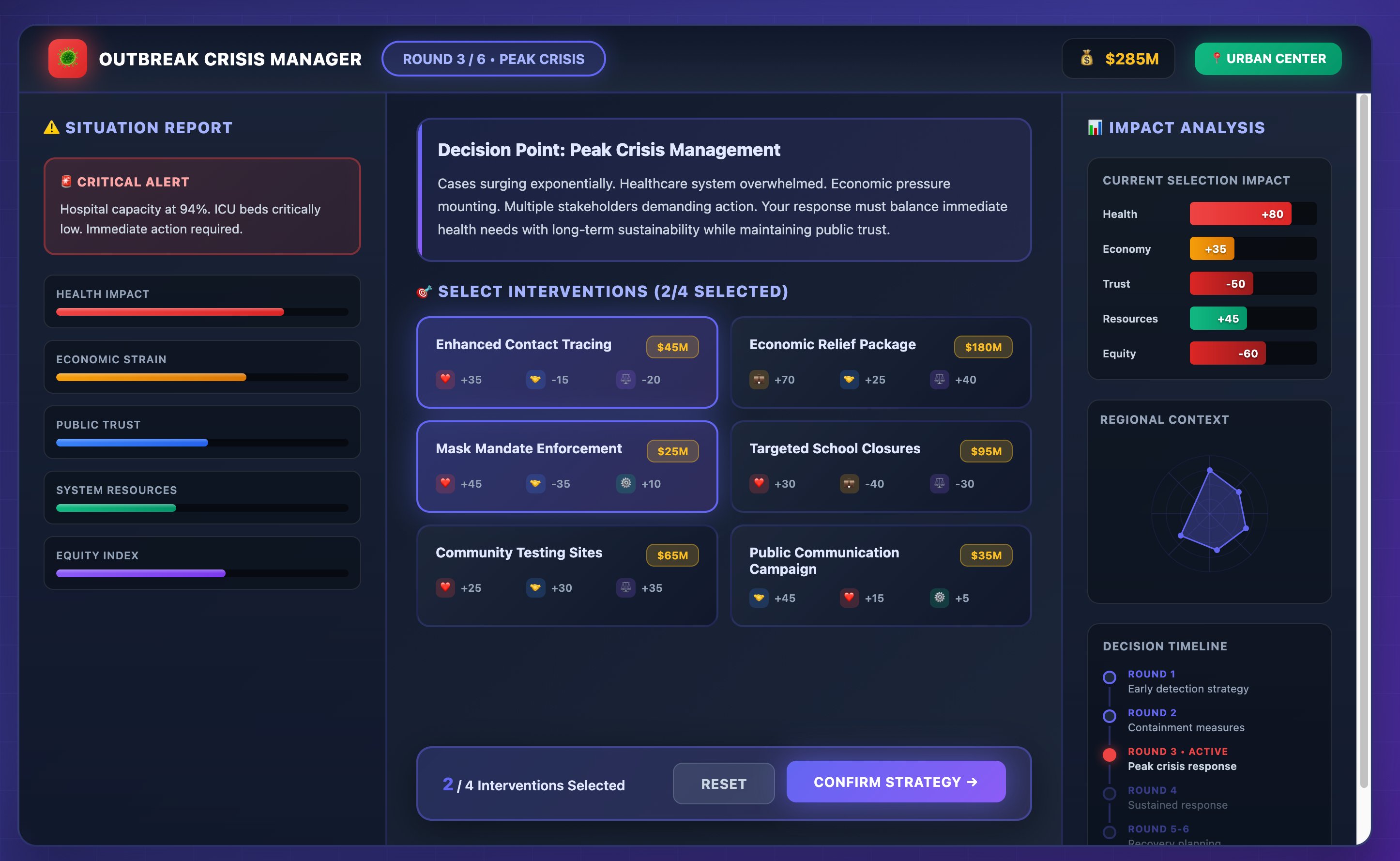
Designed for facilitated use in postgraduate teaching, professional training, and tabletop exercise settings. Regional and pathogen parameters are adaptable for different outbreak scenarios.
Interactive Exercise Series
Built as companions to The Formula for Better Health by Dr. Tom Frieden
A series of interactive exercises developed to accompany the teaching materials for The Formula for Better Health. The underlying case studies, pedagogical framework, and content are Dr. Frieden's. The contribution here is the interactive exercise architecture — the structural design that turns each case into a decision-based learning experience.
Each exercise is designed for standalone use within a structured course or workshop. Visit formulateaching.theformulaforbetterhealth.net for the full instructor resources.